APHRODITE

Welcome to the APHRODITE website
If you are taking part in the APHRODITE trial, we would like to say a huge thank you for your help in developing ways in which we can improve cancer treatments.
This website provides some useful information about the trial as follows:
- Background – what early rectal cancer is and the standard treatment for it.
- About Our Trial – summary of what the APHRODITE trial is about.
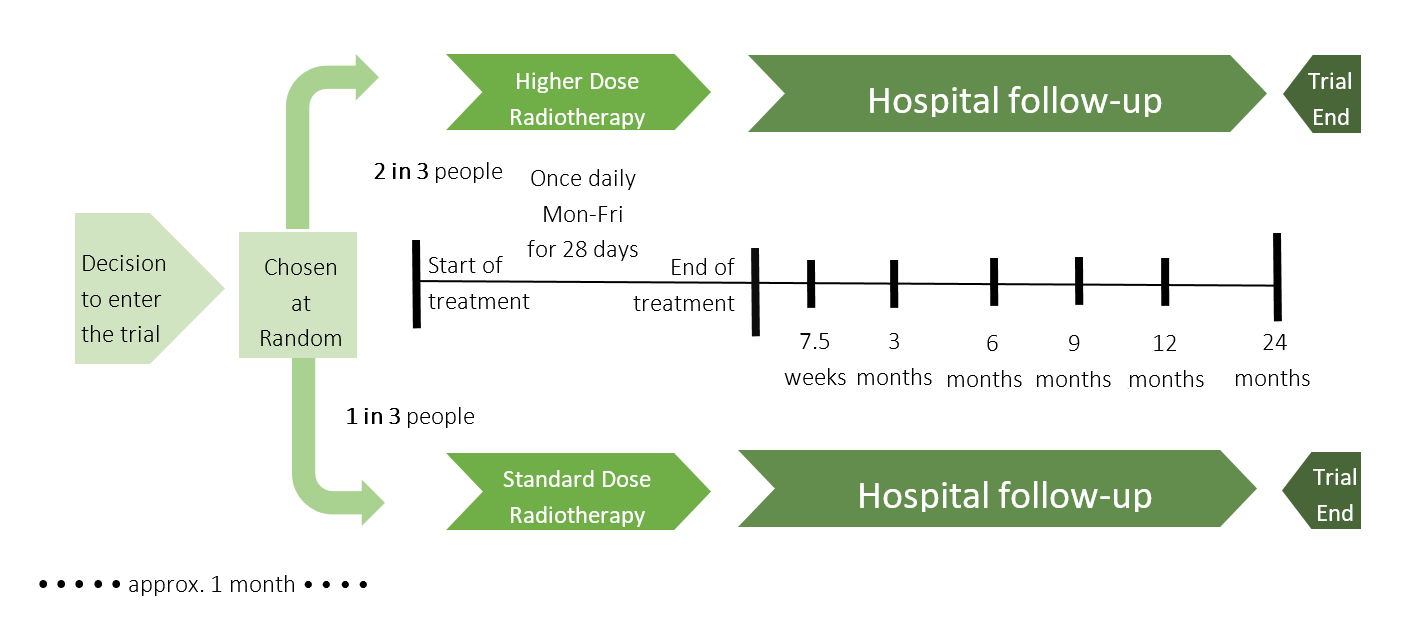
- On the Trial – what will happen to you on the trial, including a diagram of the treatment schedule.
- Documents – patient newsletters, Patient Information Sheet and Key Facts Sheet available for download.
- Meet The Team – the team working on the trial.
- Who is Responsible for the Data? – a link to who is responsible for the data on the trial.
- Useful links – links to the funder website, Leeds Radiotherapy Research Group and the trial twitter page for healthcare professionals.
- Useful information for healthcare professionals – ISRTCN and IRAS numbers, details and site specific newsletters.
Background
Patients with small rectal cancers (i.e., early back passage cancers) would normally have surgery to remove the whole rectum to treat their cancer. However, there are some patients who are not suitable for surgery or would prefer not to have surgery.
There can be multiple reasons for this. One reason is that surgery could be thought to be too risky due to other medical problems, increasing the risks of having surgery. Another reason could be that because the patient would have difficulty looking after a stoma (bowel bag) following surgery. Or it could simply be that the patient strongly prefers to explore other treatment options rather than surgery.
For these patients radiotherapy or ‘chemoradiotherapy’ can be used which just means that radiotherapy is given at the same time as chemotherapy. The radiotherapy is given over 5.5 weeks and can lead to the cancer disappearing in about one third of patients.